Physical therapy: simple steps to cut pain and get moving
Got a nagging backache, sore knee, or pelvic pain that won't quit? Physical therapy isn't just for post-surgery rehab. It can help with chronic pain, buildup of stiffness, balance problems, and pelvic floor issues. Read on for clear, useful steps you can try today and guidance on when to see a pro.
Quick wins you can try at home
Start small. Try these three exercises 1–2 times daily. Stop if pain increases and call a clinician.
1) Glute bridge — Lie on your back, knees bent, feet hip-width. Squeeze your glutes and lift hips until your body forms a straight line from shoulders to knees. Hold 2 seconds, lower slowly. Do 10–15 reps. It wakes up the hips and eases lower back strain.
2) Scapular squeezes — Sit tall. Pinch shoulder blades together and hold 3–5 seconds, then relax. Repeat 10–20 times. Great for rounded shoulders and neck pain from desk work.
3) Pelvic floor (gentle) squeeze — Imagine stopping urine midstream. Squeeze those muscles gently, hold 3 seconds, relax 5. Do 8–12 reps. Useful for bladder urgency or pelvic discomfort, but check with a therapist if you have pain doing them.
When to see a physical therapist and how to choose one
See a therapist if pain lasts more than 4–6 weeks, limits daily tasks, or comes with numbness, weakness, fever, or sudden weight loss. A good therapist will ask about your history, watch how you move, and give a clear plan with measurable goals.
How to pick one: check credentials (licensed PT or physiotherapist), read reviews, and choose someone who explains things simply and teaches self-management. If you need pelvic floor work, look for someone with pelvic health training. For sports injuries, ask about experience with athletes.
Expect hands-on work, guided exercises, and homework. Most programs mix manual therapy, targeted strengthening, and mobility drills. Good therapists teach you to avoid flare-ups and progress safely.
Extra tips: use ice for sharp inflammation and heat for stiff muscles, keep moving in gentle ranges, and track progress—note pain levels and what activities improve. If an online guide or pharmacy question pops up, look for trusted sources and verify treatment suggestions with a clinician.
If your issue links to another health problem—like bladder pain or persistent neurological signs—coordinate care. For example, pelvic pain often needs both medical review and targeted pelvic floor therapy. We have deeper reads on related topics across the site if you want to explore medical background along with rehab options.
Want a short exercise plan tailored to your problem? Share your main pain area and activity level, and I’ll sketch a one-week starter plan you can try safely.
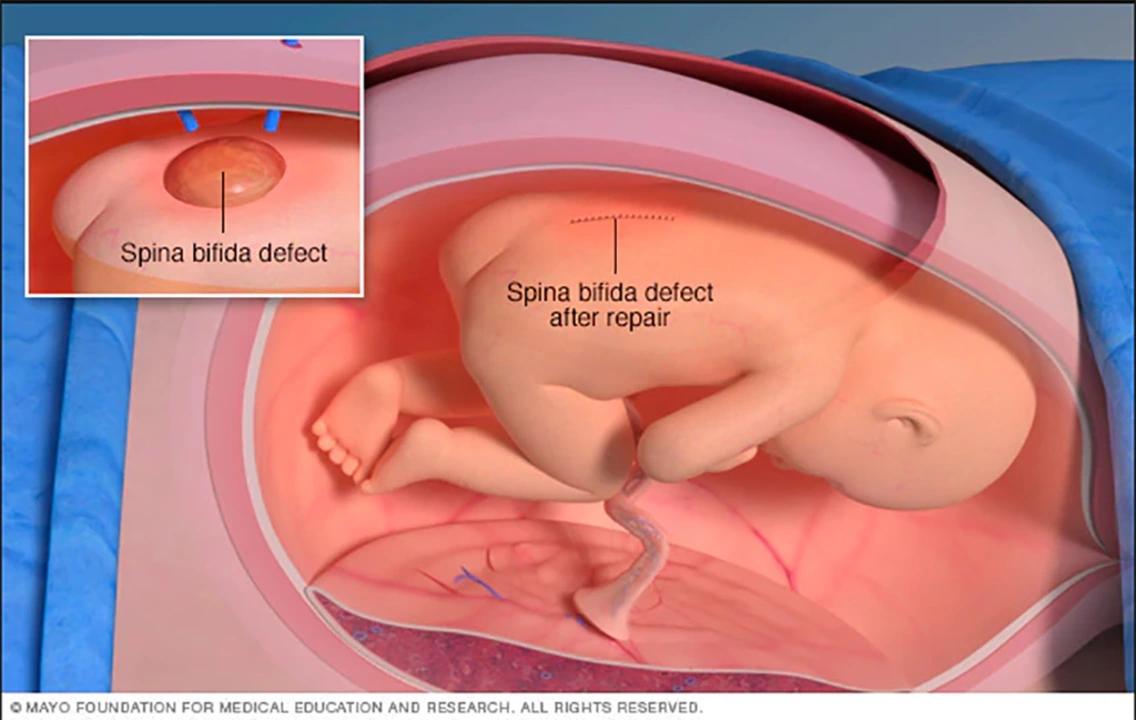
The role of physical therapy in managing spina bifida symptoms
In my latest blog post, I explored the vital role physical therapy plays in managing spina bifida symptoms. I discovered that physical therapy can greatly improve mobility, prevent complications, and enhance the overall quality of life for individuals with this condition. Additionally, I learned that early intervention is crucial for optimal results, as it helps to develop strength and flexibility in affected muscles. Furthermore, I found out that physical therapists work closely with patients to create personalized treatment plans, focusing on individual needs and goals. Overall, I believe that physical therapy is an essential component in managing spina bifida and should be considered as a crucial part of the treatment plan.
© 2026. All rights reserved.