Diabetic Bone Disease: What You Need to Know Now
If you have diabetes, you might not expect your bones to be at risk. But long-term high blood sugar can make bones weaker, slower to heal, and more likely to break. Knowing the warning signs and the steps you can take now helps you protect your bones and stay active.
What is diabetic bone disease? It’s a term that covers lower bone density, poorer bone quality, and slower fracture healing linked to diabetes. People with type 1 diabetes often show lower bone density, while people with type 2 may have normal density yet still face higher fracture risk. Both high blood sugar and diabetes-related nerve and circulation problems play a role.
How will you notice it? Common clues include fractures from minor falls, slow healing after breakage, persistent bone or joint pain, and changes in posture. If you can’t explain a broken bone or your recovery drags on, tell your doctor—early checks make a big difference.
Tests and diagnosis
Your doctor will start with a medical history and physical exam, then likely order a DEXA scan to measure bone density. Blood tests check vitamin D, calcium, kidney function, and markers of bone turnover. If you’ve had fractures or unusual bone pain, imaging like X-rays or MRI can show damage or delayed healing. Continuous glucose monitoring and A1c results help link blood sugar control to bone health.
Practical steps to protect your bones
Control blood sugar: Better glucose control lowers damage to bone cells and blood vessels that feed bone. Aim for targets set with your healthcare team and use CGM if needed.
Move more: Weight-bearing exercise—walking, stair climbing, light resistance—strengthens bone and muscle. Start slow and build up three to five times a week. Balance and fall-prevention exercises cut fracture risk.
Eat for bone health: Get enough calcium and vitamin D from food or supplements if your doctor recommends them. Foods like low-fat dairy, leafy greens, and fortified products help. Protein supports healing, so include lean protein at meals.
Check medications: Some diabetes drugs and other common meds affect bone. Ask your provider whether your prescriptions raise fracture risk and if safer options exist.
Fix falls risks at home: Remove loose rugs, add grab bars, improve lighting, and wear supportive shoes. Small changes prevent many injuries.
Treatment options: If tests show low bone density or fractures, treatments include bisphosphonates, denosumab, or anabolic drugs—your doctor will pick based on diabetes status, kidney function, and fracture history. Physical therapy and pain management speed recovery after breaks.
Keep an eye on complications: Neuropathy and poor circulation make injuries worse. Regular foot exams, smoking cessation, and blood pressure control protect both blood vessels and bones.
Talk openly with your healthcare team about bone concerns. With good sugar control, targeted exercise, proper nutrition, and the right tests, you can cut your fracture risk and keep moving strong.
Schedule a bone health review if you’re over 50 or have had diabetes for many years—early action prevents problems.
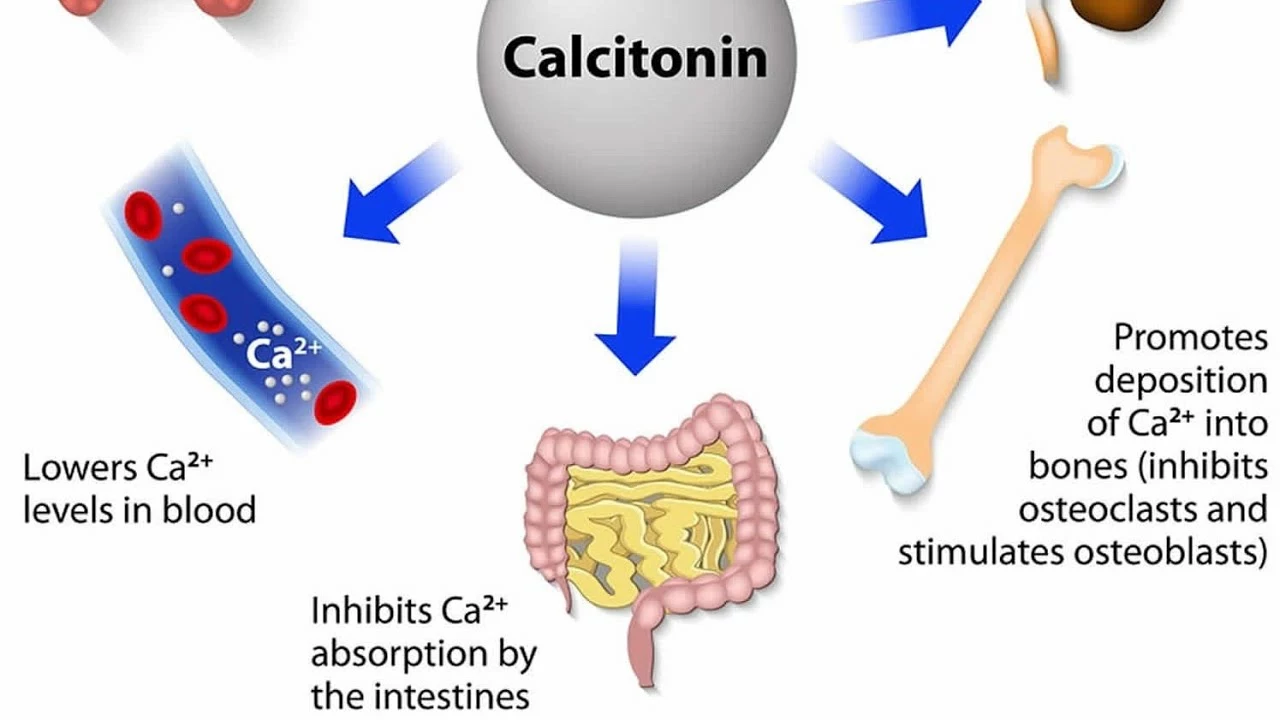
The potential role of calcitonin in managing diabetic bone disease
Hey there, fellow health enthusiasts! So, I've been diving deep into the fascinating world of diabetes management and guess what? Our good old friend calcitonin might just be the new superhero in town. This hormone, usually chilling in our thyroid gland, could be the key to managing diabetic bone disease. Who knew, right? It might just be the 'bone-saver' we've been looking for, helping to maintain bone strength and health. So, here's a cheer for calcitonin, potentially our next big weapon in the fight against diabetes-related bone disease!
© 2026. All rights reserved.